If you picture a person grappling with anxiety, you might imagine a stressed young adult or an overwhelmed mid-career professional navigating modern burnout. Yet, mental health data paints a very different picture. Recent global estimates published by the National Institutes of Health suggest that approximately 25 to 28 percent of older adults experience anxiety symptoms. Furthermore, a 2025 survey of thousands of seniors revealed that nearly one in three reported a clinical diagnosis of anxiety or depression. Despite these staggering numbers, late-life anxiety remains a chronically hidden epidemic.
Getting older is a profound transition. It requires you to navigate changes in your physical body, your social circle, and your fundamental sense of identity. It is entirely valid to feel overwhelmed by these shifts. However, living in a constant state of dread, excessive worry, or physical tension is not a required chapter of your aging story. Many older adults suffer in silence because their symptoms are misattributed to the natural aging process or dismissed as inevitable reactions to health challenges.
Understanding the unique ways senior anxiety presents itself is the first step toward reclaiming your peace of mind. Whether you are navigating these feelings yourself or trying to support a loved one, you deserve to know that relief is entirely possible; your golden years do not have to be defined by a shrinking world or persistent fear.

The Hidden Epidemic: Why Anxiety in Older Adults Goes Unnoticed
Why is such a prevalent condition so consistently missed by families and medical professionals alike? The issue of overlooked anxiety elderly populations face often stems from generational differences in how emotional distress is expressed. Many individuals currently in their sixties, seventies, and beyond grew up in an era where mental health was heavily stigmatized. Psychological struggles were often viewed as a personal failing or a lack of resilience, teaching an entire generation to suppress their emotional pain.
Consequently, older adults rarely walk into a doctor’s office and explicitly say, “I feel anxious” or “I am having panic attacks.” Instead, they are much more likely to report feeling “tense,” “stressed,” or “on edge.” They might express deep concerns about their physical health, financial stability, or the safety of their adult children. Because they do not use the modern clinical vocabulary of mental health, their genuine psychological distress frequently flies under the radar of primary care physicians.
Furthermore, the medical system itself is often fractured when treating seniors. Geriatric care heavily prioritizes physical ailments—managing blood pressure, monitoring cardiovascular health, and preventing falls. When a senior complains of fatigue or stomach pain, the immediate clinical response is to run physical diagnostic tests. If the tests come back clear, the symptoms are often chalked up to “just getting older,” leaving the underlying anxiety completely unaddressed.
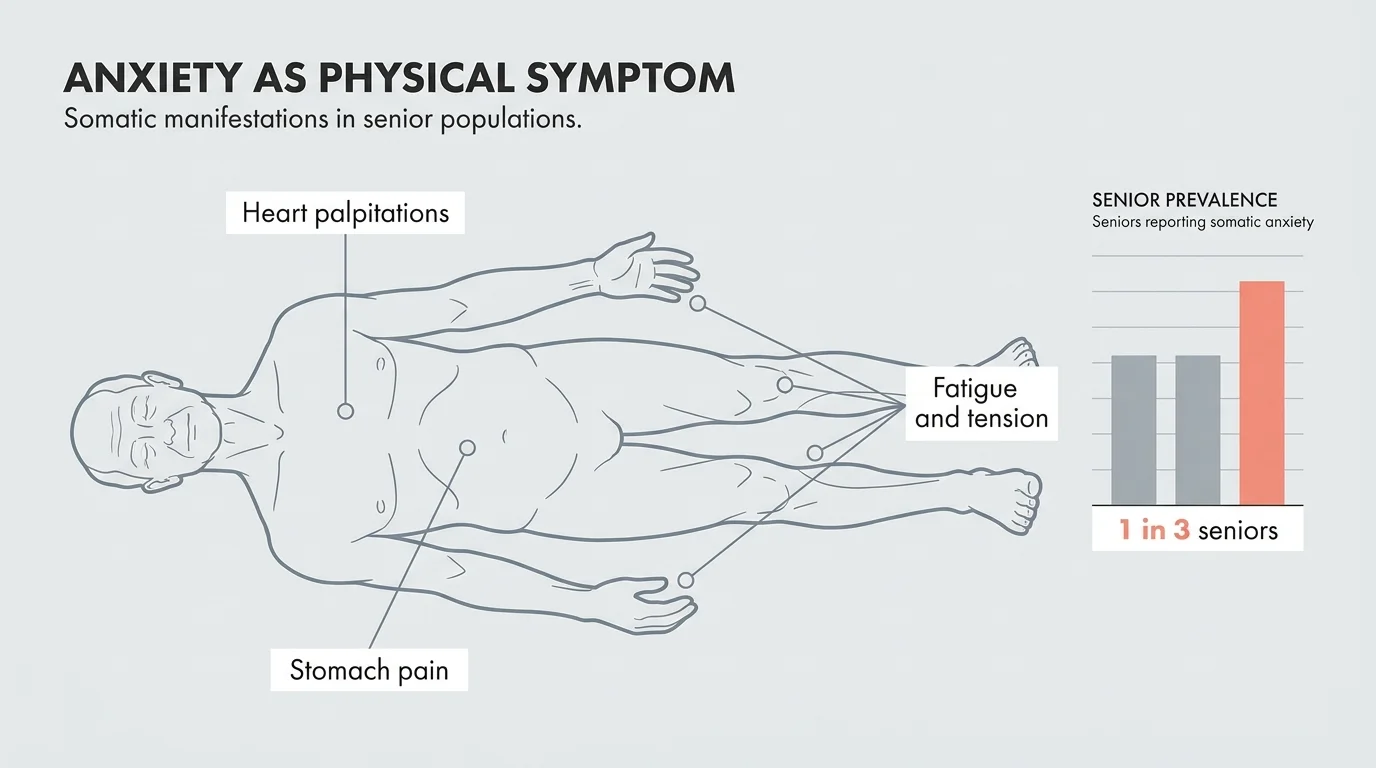
Physical Overlap: When Anxiety Masks Itself as Illness
One of the most complex aspects of mental health 60+ care is that anxiety in older adults is overwhelmingly somatic—meaning it is experienced in the body rather than just the mind. When evaluating anxiety symptoms, aging bodies often present physical rather than emotional clues. The nervous system’s fight-or-flight response triggers a cascade of physiological changes that closely mimic severe medical conditions.
This physical overlap is a primary reason anxiety goes undiagnosed. Doctors and patients alike focus on treating the bodily symptoms, entirely missing the emotional root cause. Common physical manifestations of senior anxiety include:
- Cardiovascular symptoms: Heart palpitations, a racing pulse, or a feeling of tightness in the chest are hallmark signs of anxiety that are frequently mistaken for cardiac events.
- Digestive distress: The gut and the brain are intimately connected. Anxiety often causes persistent nausea, chronic upset stomach, or sudden changes in bowel habits.
- Chronic sleep disturbances: Difficulty falling asleep, waking up unusually early, or suffering from fragmented sleep are often the very first signs of an overactive nervous system.
- Muscle tension and unexplained pain: Chronic worry causes the body to physically brace itself. This leads to tension headaches, jaw pain, and generalized muscle aches that resist standard pain relievers.
- Shortness of breath: A feeling of not being able to take a full, deep breath can trigger further panic, often leading to unnecessary pulmonary evaluations.
When physical symptoms persist despite medical clearance from your doctor, it is highly appropriate to consider whether your nervous system is stuck in a state of chronic hyperarousal.

Comparing Normal Aging Concerns with Clinical Anxiety
It is perfectly natural to worry about the realities of aging. Everyone experiences moments of stress when confronting a new medical diagnosis or transitioning into retirement. So, how do you distinguish between standard age-related concerns and a clinical anxiety disorder? The difference usually lies in the intensity, duration, and impact of the worry. Normal concerns are proportional to the situation and pass over time; clinical anxiety is persistent, intrusive, and limits your ability to live freely.
| Normal Age-Related Concern | Signs of Clinical Anxiety |
|---|---|
| Feeling nervous about the results of an upcoming medical scan or blood test. | Obsessively checking your body for signs of illness or frequently calling the doctor for reassurance despite clear test results (Health Anxiety). |
| Feeling a temporary sense of loss, boredom, or lack of direction shortly after retiring. | Experiencing a pervasive sense of dread and identity loss that prevents you from getting out of bed or enjoying past hobbies. |
| Exercising appropriate caution when walking on an icy or uneven sidewalk to avoid a fall. | Developing an intense fear of falling that causes you to avoid leaving the house entirely, even in safe and familiar environments. |
| Occasionally forgetting a word in conversation or misplacing your reading glasses. | Spiraling into panic over minor memory lapses, convinced you are developing dementia, and obsessively testing your own cognitive performance. |

Common Triggers for Senior Anxiety
Anxiety does not happen in a vacuum. The later stages of life introduce a unique set of psychosocial and biological stressors that can deeply unsettle even the most resilient individuals. Recognizing these triggers can help you understand that your anxiety is a valid response to your environment, not a personal weakness.
The Fear of Cognitive Decline
According to the American Psychological Association, one of the most profound fears among older adults is the loss of cognitive function. “Dementia phobia” is a specific form of health anxiety where an individual becomes hyper-fixated on their memory. Because anxiety itself clouds thinking, reduces concentration, and causes memory lapses, it creates a cruel feedback loop: you worry about your memory, the anxiety makes you forgetful, and the forgetfulness deepens your panic.
Loss of Independence and the Fear of Falling
Mobility changes represent a significant threat to personal autonomy. A fear of falling is incredibly common and highly restrictive. While it stems from a valid desire for self-preservation, this fear often leads older adults to severely restrict their physical activity. Ironically, this lack of activity leads to muscle deconditioning, which actually increases the risk of falls—further exacerbating the anxiety.
Biological and Medication Triggers
As you age, your neurobiology shifts. Research indicates that levels of certain neurotransmitters responsible for regulating mood, such as serotonin, can decrease naturally over time. Additionally, older adults often manage multiple chronic conditions, leading to “polypharmacy” (the use of multiple medications). Certain drugs—including thyroid medications, asthma inhalers, corticosteroids, and even some over-the-counter cold medicines—can produce side effects that mimic or trigger severe anxiety.

The Impact of Social Isolation and Grief
The landscape of your social world changes as you age. Retirement removes the daily built-in socialization of the workplace. Children move away and build their own busy lives. Most profoundly, later life inevitably involves the loss of peers, siblings, and spouses. Grief is a heavy burden, and when multiple losses occur in rapid succession—often referred to as “bereavement overload”—the nervous system can become entirely overwhelmed.
Social isolation is one of the most potent catalysts for late-life anxiety. When you spend vast amounts of time alone, you lack the external distractions and social mirroring that help regulate mood. A quiet, empty house provides fertile ground for the mind to ruminate on fears and “what-if” scenarios. Without someone to reality-check your worries or provide comforting physical touch, minor concerns can quickly snowball into catastrophic thinking.
“If there is meaning in life at all, then there must be meaning in suffering.” — Viktor Frankl, Psychiatrist and Holocaust Survivor
Processing grief and combating isolation requires finding new avenues for meaning. When you lose the roles that previously defined you—such as an active career or primary caregiver—anxiety often rushes in to fill the void. Seeking out new purpose, whether through community volunteering, joining a support group, or engaging in legacy-building projects with your family, is a vital component of protecting your psychological well-being.

Myths Worth Debunking
To advocate effectively for yourself or your loved one, we must clear away the cultural misconceptions surrounding aging and mental health. These myths prevent millions of older adults from receiving the care they desperately need.
Myth 1: Anxiety is just a normal part of getting older.
While aging brings unique challenges, living in a constant state of fear is never normal. The National Institute of Mental Health asserts that anxiety disorders are highly treatable medical conditions, not inevitable milestones of aging. Accepting anxiety as “normal” robs you of the opportunity to improve your quality of life.
Myth 2: Seniors are “too set in their ways” for therapy to work.
There is a pervasive, ageist assumption that older adults cannot learn new coping skills. This is biologically and psychologically false. Neuroplasticity—the brain’s ability to form new neural connections—continues until the end of life. Older adults frequently excel in therapy because they bring decades of lived experience, patience, and perspective to the therapeutic process.
Myth 3: Getting help just means being medicated into a stupor.
Many seniors fear that psychiatric help will result in being prescribed heavy sedatives that will alter their personality or cause cognitive impairment. In reality, modern geriatric mental health care focuses heavily on talk therapy, lifestyle adjustments, and, if necessary, carefully calibrated, low-dose medications that support clarity rather than diminish it.

Signs It’s Time to Talk to a Therapist
It can be difficult to know when everyday worry has crossed the line into a condition that requires professional support. You do not need to wait for a crisis to seek help. Consider speaking to a licensed therapist or counselor if you recognize any of the following scenarios in your life:
- Your world is shrinking: You frequently cancel social plans, avoid leaving the house, or stop engaging in hobbies you once loved because the anticipation of what might go wrong feels too overwhelming to bear.
- Your physical symptoms have no medical cause: You have undergone cardiac, gastrointestinal, or neurological exams for your physical discomfort, but your doctors consistently tell you that your tests are clear and your body is physically stable.
- Your sleep is fundamentally disrupted: You regularly lie awake for hours, trapped in a cycle of rumination about your health, your family, or your finances, leaving you exhausted and foggy the next day.
- You feel a profound sense of paralysis: Daily tasks, such as opening the mail, paying bills, or making simple decisions about what to eat, feel like insurmountable mountains due to a paralyzing fear of making a mistake.

Evidence-Based Treatments: What Actually Works
Finding help for seniors anxiety is highly possible, and the outcomes are incredibly promising. Research evaluating the efficacy of psychological treatments for older adults demonstrates that therapies are highly effective, sometimes achieving remission rates of over 60 percent for anxiety disorders.
Cognitive Behavioral Therapy (CBT)
CBT is the gold standard for treating anxiety. It operates on the principle that our thoughts, feelings, and behaviors are interconnected. A CBT therapist will help you identify catastrophic thought patterns (e.g., “If I get a headache, it must be a stroke”) and gently challenge them with realistic evidence. For older adults, CBT is often adapted to include “Pleasant Activity Scheduling”—a behavioral technique that encourages engaging in one joyful or meaningful activity a day to combat isolation and break the cycle of worry.
Acceptance and Commitment Therapy (ACT)
ACT is particularly powerful for seniors because it acknowledges that some stressors—like chronic pain or the loss of a spouse—cannot be “fixed” or changed. Instead of fighting the reality of these hardships, ACT teaches psychological flexibility and mindfulness. It helps you accept unavoidable pain while simultaneously committing to actions that align with your core values, allowing you to live a rich, meaningful life alongside your physical or emotional challenges.
Pharmacological Support
When medication is necessary, doctors often prescribe Selective Serotonin Reuptake Inhibitors (SSRIs) or Serotonin-Norepinephrine Reuptake Inhibitors (SNRIs). Because older metabolisms process medications differently, geriatric psychiatry operates on the golden rule of “start low and go slow.” When monitored carefully, these medications can lower the physiological volume of anxiety enough to allow you to engage effectively in talk therapy.
“When a person realizes he has been heard, his eyes moisten. I think in some real sense he is weeping for joy. It is as though he were saying, ‘Thank God, somebody heard me. Someone knows what it’s like to be me.'” — Carl Rogers, Psychologist and Founder of Person-Centered Therapy

How to Advocate for Yourself at the Doctor’s Office
Because the medical system can be rushed and fragmented, you must become a proactive advocate for your own mental health. When preparing for a doctor’s appointment, write down your symptoms in advance. Be explicitly clear about your emotional state. Instead of just saying, “My stomach hurts,” you might say, “My stomach hurts constantly, and I am also experiencing overwhelming worry that prevents me from sleeping or enjoying my life.”
Ask your primary care physician for a comprehensive medication review. Bring all of your prescription bottles, over-the-counter supplements, and vitamins to your appointment. Ask directly: “Could any of these medications, or the combination of them, be contributing to my feelings of anxiety or a racing heart?”
If you feel dismissed by your doctor or told that your feelings are “just a normal part of your age,” seek a second opinion. You have the right to request a referral to a geriatric psychiatrist or a licensed clinical social worker who specializes in older adults. You deserve a care provider who listens deeply and treats your psychological health with the same urgency as your physical health.

Finding Meaning and Moving Forward
Navigating late-life anxiety requires patience, self-compassion, and the willingness to ask for support. It takes immense courage to admit that you are struggling, especially if you have spent your entire life being the strong, dependable anchor for your family. However, vulnerability is not a weakness; it is the gateway to connection and healing.
By recognizing the physical and emotional signs of senior anxiety, you take the crucial first step toward reclaiming your daily joy. Whether you start by confiding in a trusted family member, reviewing your health with your primary care doctor, or reaching out to a therapist who understands the nuances of aging, remember that relief is within reach. You have survived decades of life’s challenges, accumulating profound resilience along the way. You deserve to experience this current chapter of your life with clarity, connection, and deep comfort.
This is educational content based on psychological research and general principles. Individual experiences vary significantly. For personalized guidance, consult a licensed therapist, psychologist, or counselor.











Leave a Reply